The latest CRISPR-Cas technology has been used to eliminate all traces of HIV from infected cells in the lab. Here we look at how gene editing could revolutionise clinical treatments and ask what the limitations are for its future use.

At a glance
- CRISPR-Cas gene-editing technology has been used to eliminate all traces of HIV from infected cells in the laboratory.
- Many say that more research is needed before CRISPR-based genome editing can be used more generally.
- Regulations must be developed through extensive consultation at all levels of society to ensure genome-editing technologies aren’t misused.
In the four years since Emmanuelle Charpentier and Jennifer Doudna won the Nobel Prize in Chemistry for inventing CRISPR-Cas9 technology, genome editing has advanced considerably. In new research, a paper published for the ESCMID Global (formerly known as ECCMID) annual congress in Barcelona, CRISPR-Cas has been shown to eliminate all traces of HIV from infected cells in the laboratory.
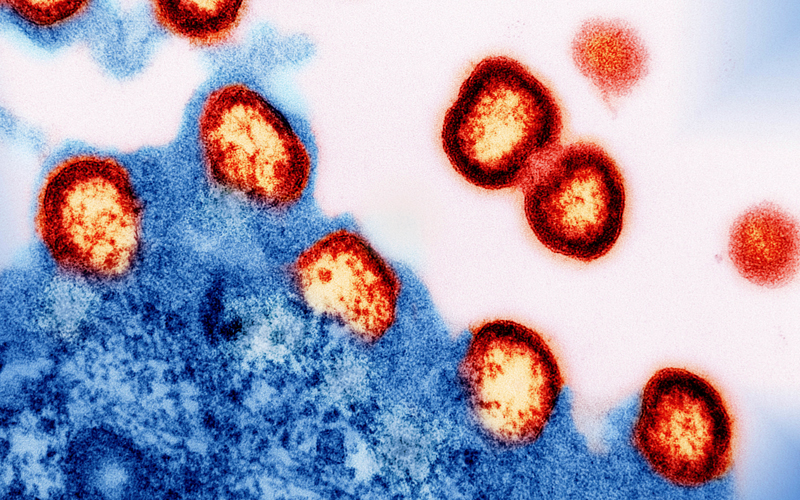
The research calls attention to the virus’ ability to integrate its genome into hosts’ DNA – infecting different types of cells and tissues in unique environments with differing characteristics. This makes it extremely difficult to eradicate and, despite the efficacy of potent antiviral drugs, HIV can rebound from established reservoirs when treatment is halted.
Led by Dr Elena Herrera Carrillo, Associate Professor in Molecular Virology and Gene Therapy at Amsterdam University Medical Center, the research used CRISPR-Cas and two guide RNAs (gRNAs) in vitro to edit “conserved” HIV sequences. These parts of the virus genome stay the same across all known HIV strains. By focusing on these conserved sections, the researchers could provide a broad therapy that eradicated multiple HIV variants across various cellular environments, and they were able to eliminate HIV from infected T cells. “We’ve demonstrated that therapeutics can be specifically delivered to the cells of interest,” Dr Herrera Carrillo says.
“These findings are crucial steps toward formulating an effective cure strategy. However, our current primary challenge lies in delivering CRISPR-Cas antivirals to HIV reservoir cells. Major vector production and delivery issues impede swift translation to animal and clinical studies.”
Targeted precision
By trialling various techniques to reduce the size of the vector delivering the CRISPR-Cas reagents into the cells, the team was able to target “hidden” HIV reservoir cells, focusing on specific proteins found on their surfaces (CD4+ and CD32a+). “We’ve made progress,” Dr Herrera Carrillo adds. “However, targeting all reservoir cells where HIV hides is a daunting task. The absence of exclusive receptor markers for these cells adds further complexity to the targeting process.”
The research also compared different CRISPR-Cas systems for their efficiency in inactivating the provirus. One system – SaCas9 – showed “outstanding antiviral performance”, by completely inactivating HIV with a single gRNA and excising the viral DNA with two gRNAs.
“What surprised us most, while studying not only Cas9 nucleases but also Cas12, is that the cleavage and subsequent repair of the double-strand break by the cell repair mechanisms differ significantly from nuclease to nuclease,” Dr Herrera Carrillo says.
The next step for this research is to optimise the delivery route to target the majority of the HIV reservoir cells. “We will combine the CRISPR therapeutics and receptor-targeting reagents and move to preclinical models to study in detail the efficacy and safety aspects of a combined cure strategy,” Dr Herrera Carrillo adds.
Improving efficacy and specificity
Since joining Amsterdam UMC, Dr Herrera Carrillo has focused her research on gene therapy strategies aimed at combating HIV infection, but she has also investigated CRISPR-Cas targeted at the SARS-CoV-2 RNA genome. “Apart from its role in genome editing, CRISPR-Cas technology is also applied in diagnostics. For example, it can be employed to detect specific genetic mutations associated with diseases and to identify pathogens in clinical samples,” she says.
In December 2023, the US Food and Drug Administration approved Casgevy and Lyfgenia (and the European Medicines Agency approved Casgevy), to use CRISPR-Cas9 to treat transfusion-dependent β-thalassemia and severe sickle cell in patients above the age of 12 who are suitable for haematopoietic stem cell transplantation but have no donor available.
“Most of the advancements in CRISPR-Cas research methods have aimed to improve the efficacy and specificity of genome editing, reducing the chance of creating unintended genetic alterations”, says Dr Gregorio Alanis-Lobato, Principal Computational Biologist at Boehringer Ingelheim.
“We’ve made progress. However, targeting all reservoir cells where HIV hides is a daunting task”
“Some examples of these efforts include using Cas orthologues other than Cas9, engineering novel nucleases, using non-homologous end joining (NHEJ) inhibitors to promote the use of the high-fidelity homology-directed repair (HDR) or avoiding double-strand breaks (DSBs) altogether with different strategies like base or prime editing,” he says.
A preventative paradigm
Biotechnology company Scribe Therapeutics builds CRISPR, genome-editing and other types of genetic modification technologies for different conditions, including cardiometabolic disease. It also has partnerships with pharmaceutical companies Lilly and Sanofi to develop CRISPR technology to treat neurological and neurodegenerative disorders and sickle cell disease, respectively.
“We have a core system called CasX that’s less than 5% identical to Cas9, which we’ve engineered from not being able to edit the human genome to editing it at potencies that are equivalent to if not exceeding what we are able to do with Cas9,” says Dr Benjamin Oakes, Scribe’s CEO and formerly an Entrepreneurial Fellow at Jennifer Doudna’s Innovative Genomic Institute.
“We’re learning more and more about the genetic underpinnings of people who have cardiovascular diseases, and hopefully we are moving from a treatment paradigm to a prevention paradigm. I would not be surprised if we could cut those numbers [of people with cardiovascular disease] in half with the proper therapies that people stay on,” he adds.
What is CRISPR-Cas?
Clustered Regularly Interspaced Palindromic Repeats (CRISPR) is a natural segment of the genetic code found in the immune system of most bacteria and archaea. It has short, repeated sequences that allow the immune system to remember and counter other organisms, such as bacteriophages.
Each repetition is followed by spacers – fragments of viral DNA from viruses that have previously tried to attack the cells. Cas proteins can unwind foreign DNA and establish whether it complements the 20 base pair spacer region of the gRNA. Spacers are transcribed into RNA molecules that guide the Cas proteins to recognise and cleave specific sequences of viral DNA upon subsequent infections.
With the guidance of the RNA, CRISPR-Cas gene editing functions like molecular scissors, and cuts the DNA at designated spots, either deleting unwanted genes, or inserting new or replacing genetic material into an organism’s cells. It allows researchers to precisely modify DNA sequences in living organisms.
Limitations

But Dr Oakes sounds caution that even newer technologies such as base or prime editing that allow more precise genetic modification only “get it right half the time, and often install other mutations that you don’t want as well”. “We believe that molecular engineering is what will enable us to overcome these limitations, but that requires time, effort and energy, and not rushing forward with some of these newer technologies without fully understanding them first,” he adds.
For Dr Alanis-Lobato, safety is the main concern. “I was happy to see the approval of Casgevy and Lyfgenia in December last year but even though there was no evidence of DSB-induced genotoxicity in the DNA of trial participants who received these CRISPR-based therapies, the possibility of undesired genomic damage cannot be completely ruled out,” he says. “It’s crucial to follow up the long-term safety profile of people receiving these therapies to inform other clinical trials and research programmes.”
He believes more research to improve the efficiency of HDR is needed before CRISPR-based genome editing can be used more generally. “The second challenge is the size of the components of the CRISPR-Cas system that must be ferried into the target cells. In many contexts, the components are just too big to be delivered effectively,” he adds. “Finally, there’s the problem of achieving tissue specificity in disorders where only one cell type or only infected cells must be targeted by the CRISPR-Cas system. It was nice to see that the work by the Herrera Carrillo group included experiments to investigate the latter two issues.”
Delivery methods for CRISPR-Cas components to target cells, particularly in vivo, represent a significant barrier, says Dr Herrera Carrillo. “Viral vectors and nanoparticles, for example, come with concerns over specificity and potential adverse side effects, including immunogenicity. Addressing these delivery challenges is essential for ensuring safe and precise genome editing.”
But the field is quickly advancing, she adds: “More precise nucleases and delivery methods are being developed and are evolving at an unprecedented speed.”
EXPLORE FURTHER
ESCMID Global website: escmid.org/congress-events/escmid-global
Biomedical Scientist interview with Jennifer Doudna: bit.ly/49vYk8b
IBMS-accredited human genome engineering course: bit.ly/3Jd0EWY
Future uses
Scribe is also developing epigenetic modification technologies that durably – but not permanently – modify the expression of the genome. “If we want to turn off a gene we can do so, but we can go back into the future and turn that gene back on,” Dr Oakes says.
But the focus must be on understanding and characterising systems and engineering them, not “digging around in the metagenome, trying to find new things and then running with them, if we really want to get to a world where we can move towards treating public health issues more broadly and preventing diseases in patients, rather than just treating rare genetic diseases”, he says.
For Dr Alanis-Lobato, one of the most exciting possibilities will be understanding how life works. “With efficient and precise genome editing it will be possible to systematically perturb gene circuits in the lab and study how cells react to these interventions across the tree of life,” he adds. “It is important to stress though that regulations must be developed through extensive consultation at all levels of society in international fora. This will ensure that genome-editing technologies aren’t misused.”
For now, Dr Herrera Carrillo and her team’s results demonstrate a “pivotal advancement towards designing a cure strategy” for HIV, she says. “We hope to achieve the right balance between efficacy and safety. Only then can we consider clinical trials in humans to disable the HIV reservoir. While these preliminary findings are very encouraging, it is premature to declare that there is a functional HIV cure on the horizon.”
1944 - DNA-mediated genetic transformation for pneumococcus is first recorded. Previously, proteins were thought to carry genetic information.
1953 - Francis Crick and James Watson confirm the double helix structure of DNA.
1961 - Marshall Nirenberg discovers how RNA transmits messages in DNA.
1962 - Waclaw Szybalski and Elizabeth Szybalska demonstrate stable genetic modification of mammalian cells. Waclaw Szybalski coins the term “gene therapy”.
1968 - Stanfield Rogers and Peter Pfuderer show how foreign genetic material can be transferred into cells by virus.
1977 - Frederick Sanger develops dideoxy nucleotide chain-termination and sequences DNA for the first time using the chain termination method.
1983 - Kary Mullis invents the polymerase chain reaction (PCR) method, which allows a small amount of DNA to be copied in large quantities over a short period of time.
1986 - Yoshizumi Ishino detects CRISPRs for the first time when analysing the gene responsible for isozyme conversion of alkaline phosphatase in E. coli.
1993 - Francisco Mojica observes that the repeat sequences are not disparate as previously thought, but a common set of features.
2002 - Ruud Jansen, Jan van Embden, Wim Gaastra and Leo Schouls identify several genes as being strictly associated with CRISPR.
2003 - The Human Genome Project is declared complete after determining 92% of the base pairs of DNA in human genes.
2005 - Alexander Bolotin et al. discover novel cas genes in Streptococcus thermophilus, including one now known as Cas9.
2007 - Rodolphe Barrangou, Philippe Horvath and their team show how CRISPR systems are an adaptive immune system, which integrate new phage DNA into the CRISPR array.
2008 - John van der Oost and colleagues show that in E. coli, spacer sequences derived from phage are transcripted into small RNAs – CRISPR RNAs (crRNAs).
2010 - Sylvain Moineau and colleagues demonstrate that CRISPR-Cas9 creates double-stranded breaks in target DNA at precise positions.
2011 - Emmanuelle Charpentier and her team find that in addition to crRNA, a second small RNA exists – trans-activating CRISPR RNA (tracrRNA).
2012 - Charpentier and Jennifer Doudna find that crRNA and tracrRNA could be fused together to create a single, synthetic guide to cut any DNA molecule.
2013 - Feng Zhang adapts CRISPR-Cas9 for genome editing in eukaryotic cells, while Jennifer Doudna and George Church show how CRISPR can edit mammalian cells.
Image credit | Richard Gleed | National Institutes Of Health, Niaid Science Photo Library